Contents
Chromhidrosis
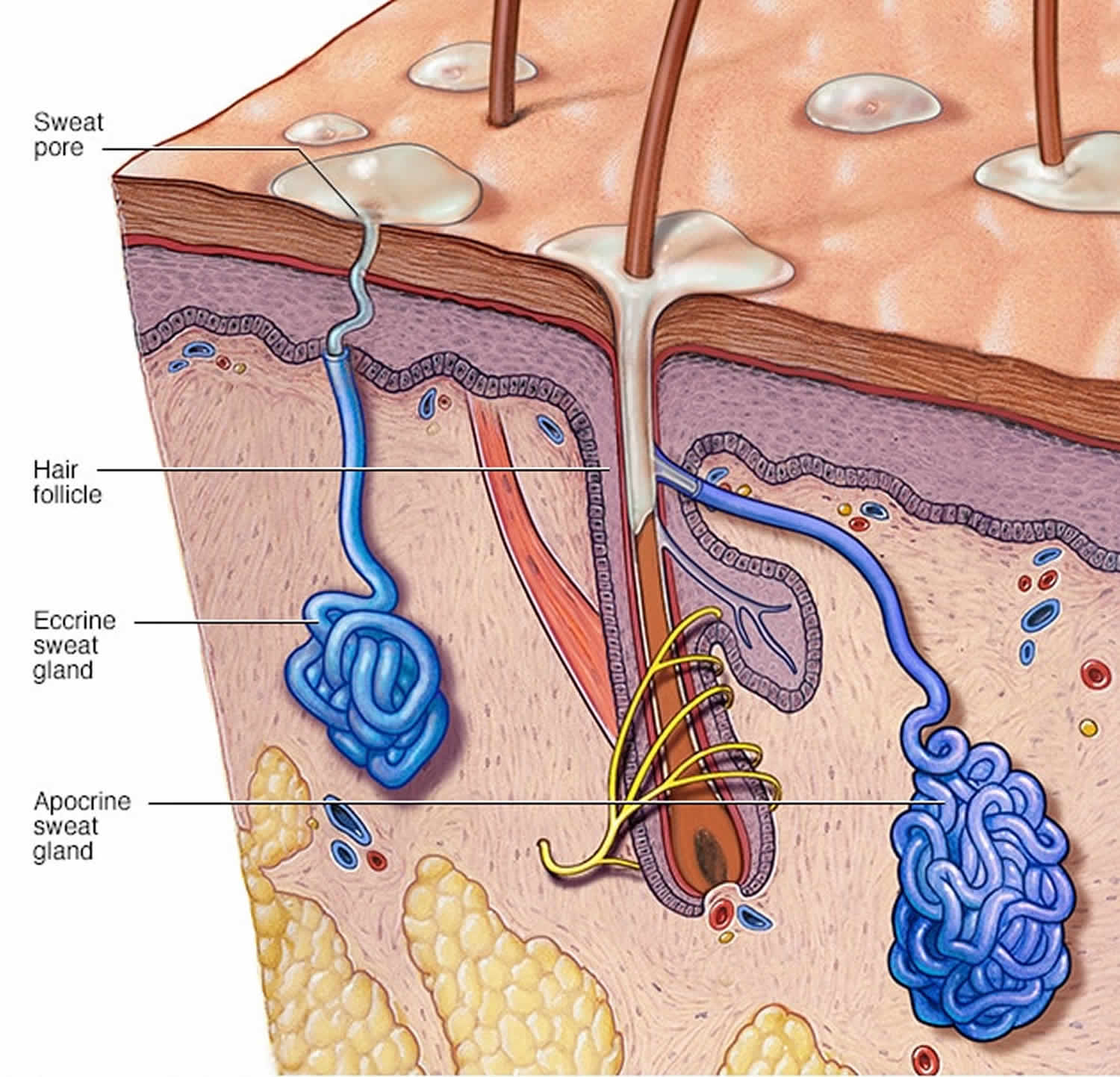
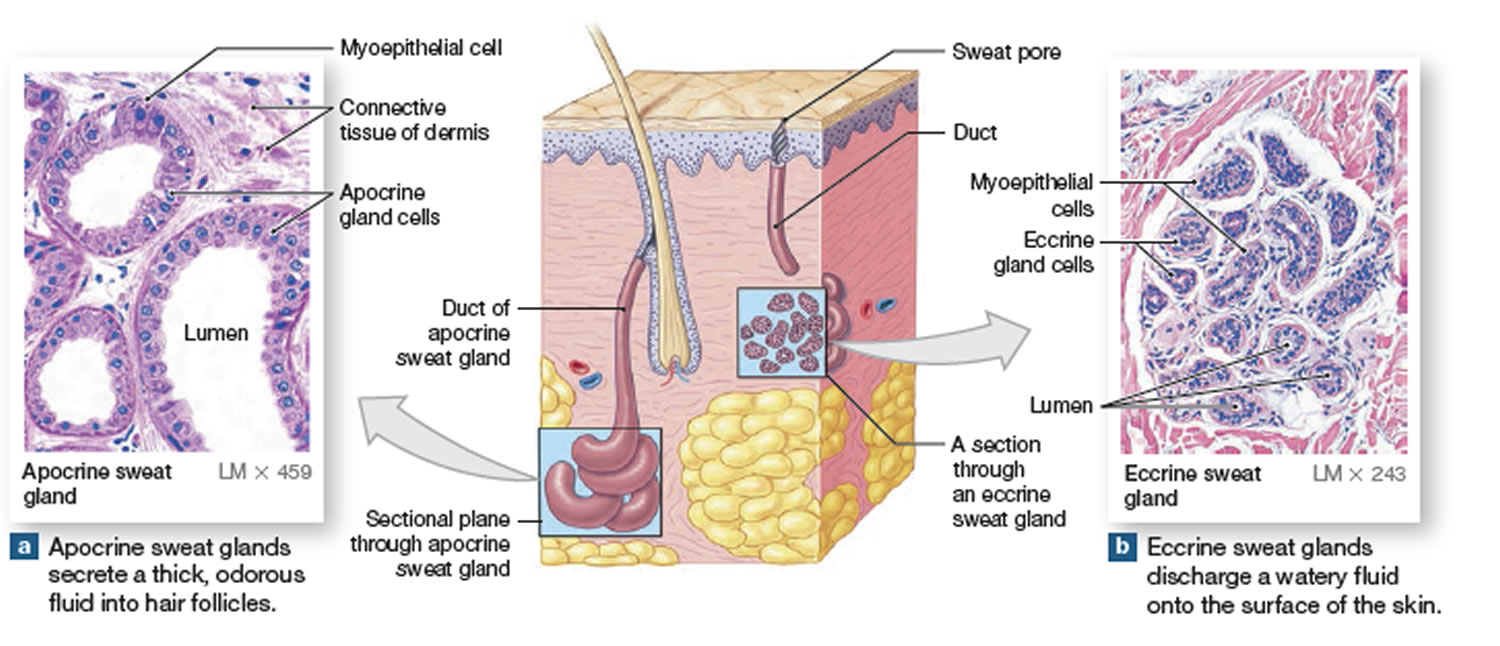
Chromhidrosis is a rare condition characterized by the secretion of colored sweat 1). Two glands produce sweat: eccrine and apocrine glands. Eccrine glands secrete a clear, odorless fluid that serves to regulate body temperature. Apocrine glands secrete a thick, milky sweat that, once broken down by bacteria, is the main cause of body odor. Normally, apocrine glands secrete scant amounts of odorless, oily fluid into the hair canal that, upon reaching the skin surface, is degraded by bacteria producing a pheromonal body odor 2).
Chromhidrosis can subdivide into three categories 3):
- Apocrine chromhidrosis: Apocrine chromhidrosis occurs in the areas where apocrine glands are present and are mostly limited to the anogenital and axillary areas, eyelids, ears, scalp, trunk, and areola. Although apocrine glands are found in the genital, axillary, areolar, and facial skin, chromhidrosis is reported only on the face 4), armpis 5) and breast areola 6). Lipofuscin pigment is responsible for the colored sweat. This pigment is produced in the apocrine gland, and its various oxidative states account for the characteristic yellow, green, blue, or black secretions observed in apocrine chromhidrosis.
- Eccrine chromhidrosis: Eccrine chromhidrosis is rare and occurs with ingestion of certain dyes or drugs. Eccrine chromhidrosis may occur almost anywhere on the body as eccrine glands are distributed with varying density throughout the skin except for the ear canal, lips, prepuce, glans penis, clitoris, and labia minora. Eccrine glands are smaller than apocrine glands, secrete a dilute salty sweat composed mainly of water and electrolytes directly onto the skin surface, and are innervated by the sympathetic nervous system. They are irregularly spaced on the epidermal ridges of the pads of the digits; however, there are no pores within the furrows. They are involved in thermoregulation, protection of the skin barrier, and excretion of electrolytes 7).
- Pseudochromhidrosis (pseudo-eccrine chromhidrosis): Pseudochromhidrosis results from the interaction of colorless eccrine sweat with extrinsic dyes, paints, or chromogenic bacteria, subsequently producing a colored sweat 8).
The yellow, green, and blue apocrine secretions produce a yellow fluorescence under a Wood lamp (UV 360 nm), whereas the dark brown and black apocrine secretions seldom autofluoresce. Substance P is also postulated to be an important neurotransmitter in this process.
Several extrinsic causes of eccrine chromhidrosis and pseudochromhidrosis include chromogenic bacteria, especially Corynebacterium species, fungi, dyes, drugs, and chemical contactants 9).
Apocrine chromhidrosis may appear at any age but usually appears after puberty, when the apocrine secretory function begins. The disease is considered chronic, however, may regress with age as apocrine secretion diminishes 10). Apocrine chromhidrosis displays no occupational or geographical predisposition and is not influenced by climatic or seasonal variation 11). There is no gender predilection, but chromhidrosis has been reported in the literature more commonly in blacks, barring facial chromhidrosis, which has been reported more commonly in whites 12). However, there are too few patients reported to draw meaningful conclusions 13).
Approximately 10% of people without chromhidrosis have colored sweat that is regarded as acceptable and within the normal range 14).
Figure 1. Sweat glands
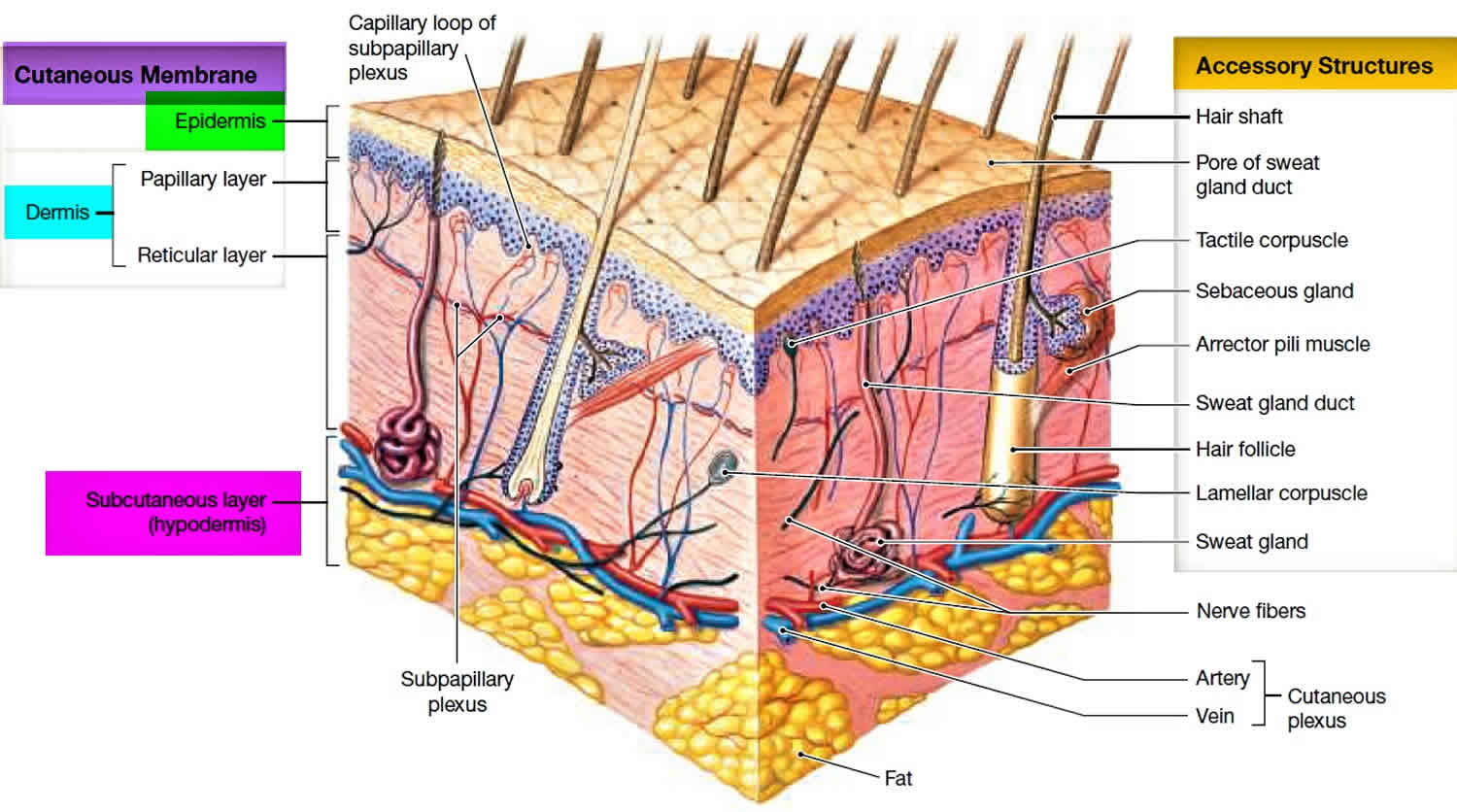
Figure 2. Skin anatomy
Chromhidrosis causes
The increased numbers of lipofuscin pigments in the secretory apocrine cells are presumed to be the cause of apocrine chromhidrosis. Lipofuscin is a yellowish brown pigment that is normally found in the cytoplasm of various organs like the relatively nondividing cells (eg, neurons) and is not specific to apocrine glands 15). In chromhidrosis, lipofuscins are found in a higher-than-normal concentration or a higher-than-normal state of oxidation in apocrine glands 16). However, why some glands experience these changes is unclear. This increased level of oxidation results in the green, blue, and even black sweat seen in chromhidrosis.
Apocrine chromhidrosis is considered an intrinsic process 17). The greater the extent of lipofuscin oxidation, the darker the lipofuscin color, which can range from yellow, green, blue, black, or brown 18). Apocrine glands are provoked by hot showers and baths, rubbing of the skin, and emotional stimuli such as pain, sexual arousal, or anxiety, which leads to the secretion of colored sweat in the case of apocrine chromhidrosis 19). Substance P may also play a role in the pathogenesis, which is why capsaicin has shown to be an effective treatment in some patients 20).
Eccrine chromhidrosis is most often caused exogenously by the coloring of clear sweat with the ingestion of water-soluble dyes such as tartrazine, heavy metals such as copper, coloring and flavoring substances in food products, and drugs such as quinines, levodopa, tartrazine-coated bisacodyl, and rifampin 21). It is caused endogenously secondarily to hyperbilirubinemia in which patients may present with a greenish hue in a palmoplantar distribution with or without pompholyx-like lesions 22).
Pseudochromhidrosis is an extrinsic process that occurs when the colorless sweat from eccrine glands subsequently develops color following exposure to exogenous influences like drugs on the surface of the skin that cause changes in the microflora on the skin surface 23). Chromogenic bacteria such as Serratia marcescens, Bacillus species, and Corynebacterium species are the most common causes. Fungi, including Malassezia furfur, dyes, paints, and chemical agents such as dihydroxyacetone, have also been implicated 24).
Chromhidrosis symptoms
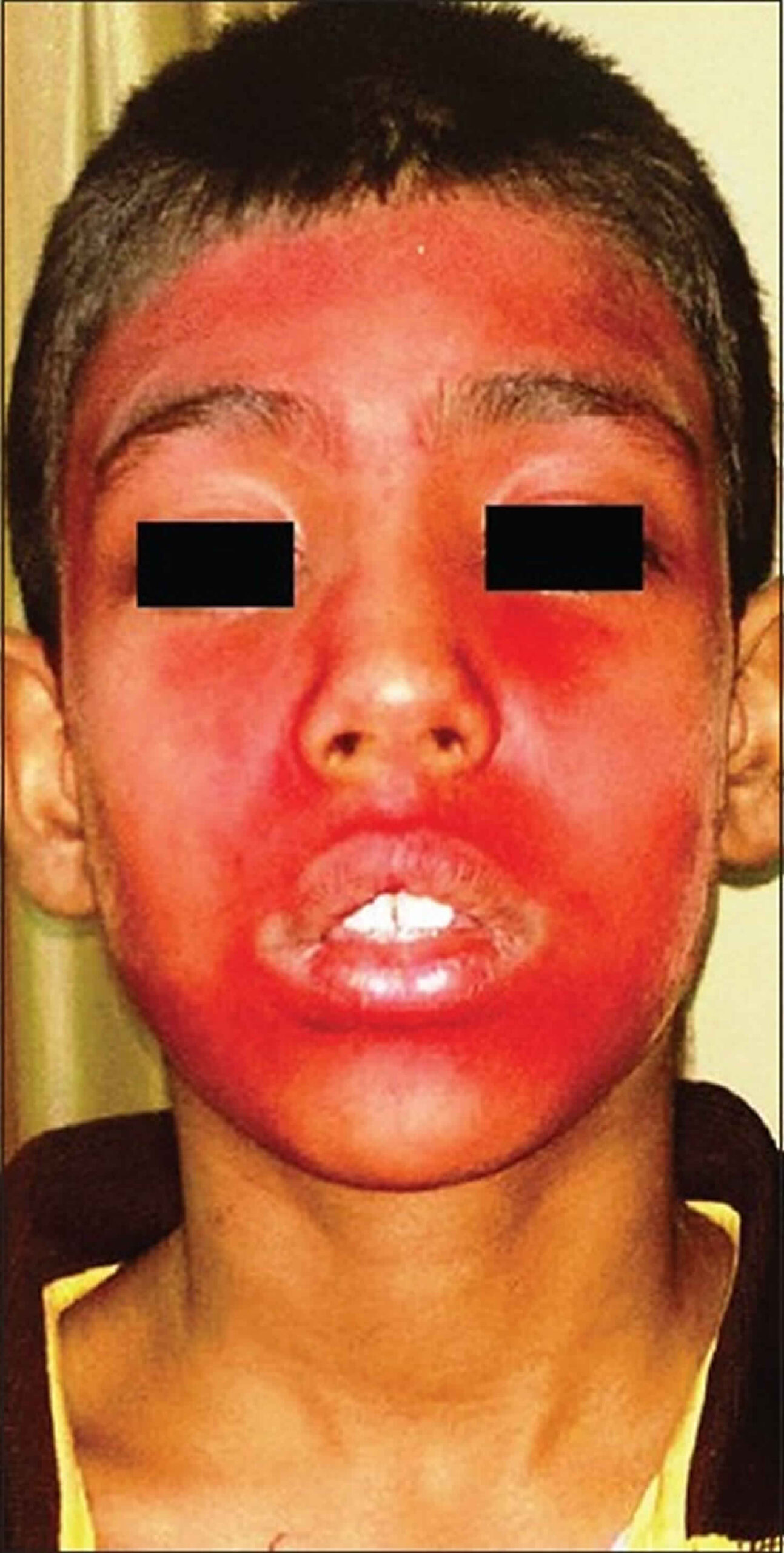
Patients with chromhidrosis will present with colored sweat, with or without staining of their clothing. Some patients may describe warmth or a prickly sensation upon emotional or physical stress preceding the appearance of colored sweat 25).
While there are no complications directly associated with chromhidrosis, there may be implications secondary to psycho-social issues 26).
Chromhidrosis diagnosis
The initial assessment should include a detailed history, including any new medications, started before the onset of chromhidrosis, including vitamins, supplements, and herbal medications 27).
While chromhidrosis is a clinical diagnosis, further studies may be needed to ascertain the type and cause of chromhidrosis if not apparent from the history and physical examination. A Wood’s lamp will fluoresce green, blue, and yellow apocrine gland secretions yellow, while black and dark brown secretions usually do not fluoresce. Skin biopsies can be sent for hematoxylin/eosin staining and fluorescence microscopy to detect and measure lipofuscins within apocrine glands 28).
Cytological examination of secretion smears may aid in detecting lipofuscin pigment within apocrine gland cells. Spectrophotometer analysis of samples from sweat, sebum, urine, skin scrapings, and extraction samples from clothing can help to aid in the diagnosis 29). Bacterial and fungal cultures of the skin may be an option to rule out pseudochromhidrosis 30). Other studies may be necessary to rule out other causes of pigmentation and include complete blood cell counts to rule out a bleeding diathesis and urinary homogentisic acid level to exclude alkaptonuria 31).
Chromhidrosis treatment
After a thorough assessment to establish the type of chromhidrosis and causality, therapy may be initiated to target the source. Apocrine chromhidrosis has no fully satisfactory cure or treatment. The treatment of apocrine chromhidrosis aims at either inducing apocrine secretion, thereby emptying the glands resulting in a temporary symptom-free period for up to 3 days, or reducing perspiration. Manual pressure can express apocrine gland contents resulting in an improved appearance for 24 to 72 hours 32). Capsaicin, applied once or twice daily, depletes the neurons of substance P and can improve the appearance in some patients 33). Burning sensation at the application site is a common side effect of capsaicin. Topical aluminum chloride and injections of botulinum toxin type A have also reportedly shown benefit in patients 34). The condition usually recurs after cessation of therapy 35).
BOTOX® injections have been attempted in 5 cases of chromhidrosis, with mixed results. BOTOX® is predominantly used to decrease eccrine sweat in persons with hyperhidrosis. However, recent reports demonstrated improvement of facial and axillary chromhidrosis with BOTOX® 36). The mechanism by which BOTOX® suppresses apocrine chromhidrosis is unclear. BOTOX® may suppress apocrine secretion by blocking cholinergic stimulation and substance P release 37).
The treatment of eccrine chromhidrosis revolves around stopping or replacing the causative agent 38).
In cases of pseudochromhidrosis, topical or systemic antimicrobials are often used to eradicate the offending microorganism. Of note, medications may have implications in altering the normal flora, allowing for chromogenic organisms to take their place 39). Discontinuation of these medications should be a consideration in such situations.
Chromhidrosis prognosis
Chromhidrosis is a benign chronic condition that may regress with time. The prognosis for chromhidrosis is good if an extrinsic cause can be identified and addressed appropriately. However, it may lead to significant anxiety, depression, or embarrassment requiring frequent clothing changes during the day 40).
References [ + ]