Contents
Biophysical profile
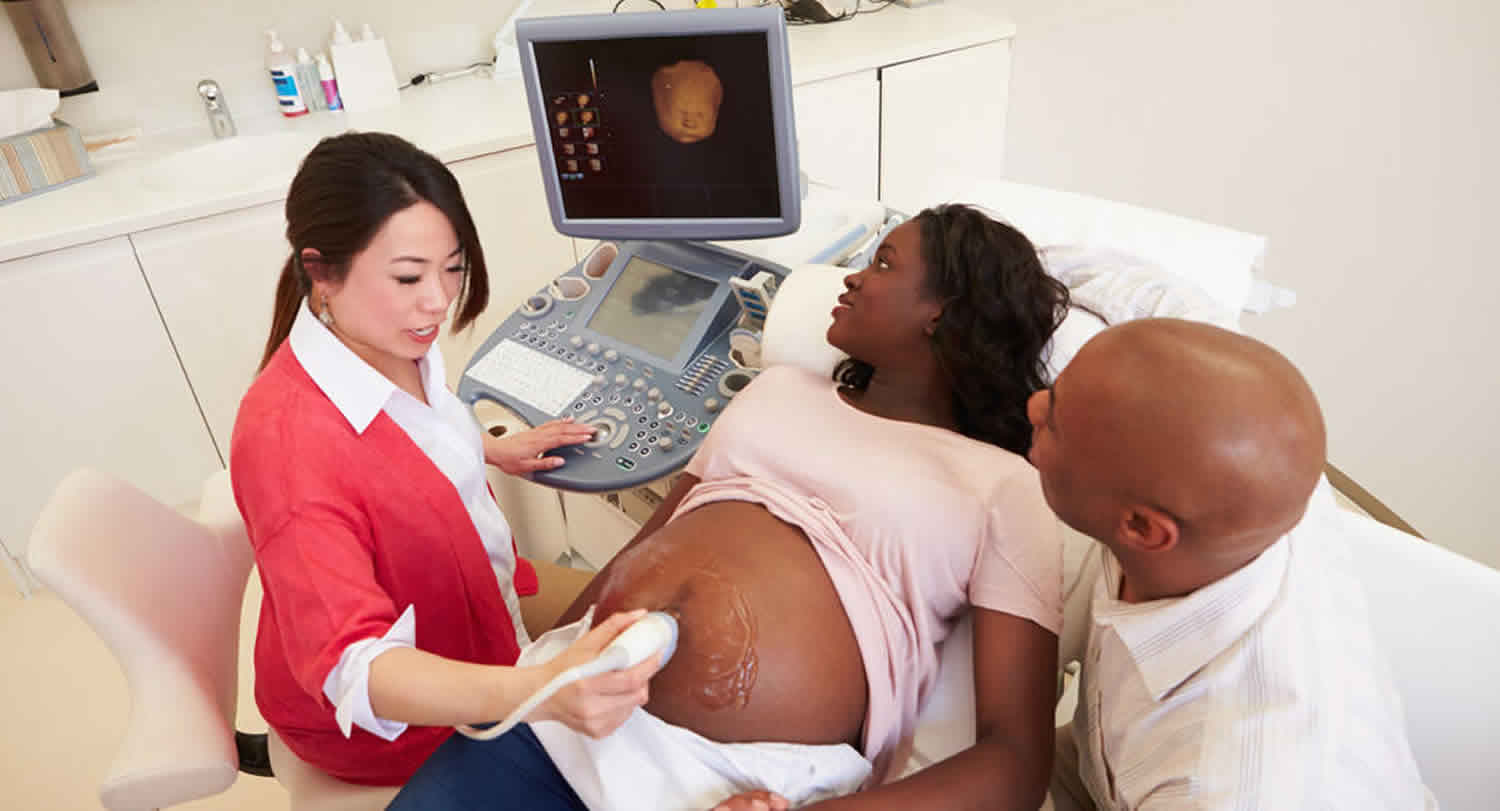
Biophysical profile also called a fetal biophysical profile, is a prenatal test used to check on your baby’s well-being. A biophysical profile is often done if there is a concern about your baby’s health. The biophysical profile test combines fetal heart rate monitoring (nonstress test) and fetal ultrasound to evaluate a baby’s heart rate, breathing, movements, muscle tone and amniotic fluid level. The nonstress test and ultrasound measurements are then each given a score based on whether certain criteria are met.
The biophysical profile combines 2 tests to check your unborn baby’s overall health: a nonstress test and an ultrasound.
- Nonstress test or electronic fetal heart monitoring. This test checks your baby’s heart rate and your contractions. This is done through devices (sensors) that are strapped to belts wrapped around your belly. Nonstress means that nothing is done to cause your baby stress during the test.
- Ultrasound evaluation. This is just like the ultrasounds done at other times during pregnancy. A healthcare provider will use an ultrasound machine to see into your uterus and check your unborn baby.
A biophysical profile test is used mainly in the third trimester to assess whether or not your baby is receiving enough oxygen and nourishment from the placenta. Biophysical profile may be considered worthwhile if:
- You have diabetes, high blood pressure or some other medical condition which could affect your baby
- You go past your due date
- Your baby appears to be small or not growing
- Your baby is less active than normal
- You have an abnormality found on ultrasound examination
- You have previously had an unexplained stillbirth or a previous small baby
Typically, a biophysical profile is recommended for women at increased risk of problems that could lead to complications or pregnancy loss. The test is usually done after week 32 of pregnancy, but can be done when your pregnancy is far enough along for delivery to be considered — usually after week 24. A low biophysical profile test score on a biophysical profile might indicate that you and your baby need further testing. In some cases, early or immediate delivery might be recommended.
A biophysical profile is a noninvasive test that doesn’t pose any physical risks to you or your baby. However, it’s not always clear that the test improves pregnancy outcomes. Find out what a biophysical profile involves and whether this prenatal test might benefit your baby.
During the biophysical profile, your provider is looking at 5 main areas to check your baby’s health: body movements, muscle tone, breathing movements, amniotic fluid, and heartbeat.
Each of these 5 areas is given a score of either 0 (abnormal) or 2 (normal). These scores are then added up for a total score ranging from 0 to 10. In general, a score of 8 or 10 is normal, while 6 is borderline. Below 6 is a sign of possible problems. More tests may be needed.
The biophysical profile test results can also help your healthcare provider decide if your baby might need to be born early.
The scientific basis of biophysical profile scoring
When a baby becomes low in oxygen it interferes with brain activity and this affects fetal heart rate patterns, fetal movement, and tone, in both animals and humans. Low amniotic fluid volumes can result from decreased fetal urine production. This is seen with low oxygen levels too, because blood flow in the baby is redistributed away from the fetal kidneys in favor more vital organs such as the brain, heart and adrenal glands. However, there are other reasons which can cause a low biophysical profile test score on the day. Fetuses naturally have sleep-wake cycles which mean that they may not demonstrate active fetal movements for up to 20 minutes, normally. So the fetus has to be examined long enough to account for these normal behaviors.
What’s the biophysical profile test procedure like?
A detailed ultrasound examination during which the sonographer will observe
- your baby’s body movements
- your baby’s muscle tone (position of flexion or extension at rest)
- your baby’s breathing movements (the baby’s ability to move his chest muscles and diaphragm) and
- the amount of amniotic fluid around the baby
It takes about 30 minutes but it may take less time if the baby demonstrates all of the activities described in quick succession.
If the baby does not show that these four features are normal, you may have to proceed to another test, called a cardiotocograph (CTG).
What is a cardiotocograph (CTG)?
A CTG (cardiotocograph) test assesses whether your baby’s heart rate changes when it is moving.
For this, you sit comfortably on a couch and have two transducers in contact with your tummy for about 20 minutes.
One monitors your baby’s heartbeat (cardio), the other records contractions in your uterus (toco).
You will be asked to press a button when you feel a fetal movement. It is then recorded on a graph while you read a magazine and relax.
How do I get ready for a biophysical profile?
You don’t have to do anything to get ready for a biophysical profile. The test will likely be done in your healthcare provider’s office. No hospital stay is needed. A biophysical profile is typically done after 32 to 34 weeks of pregnancy.
Why is fetal biophysical profile test done?
A biophysical profile is used to evaluate and monitor your baby’s health. The goal of a biophysical profile is to prevent pregnancy loss and detect a low oxygen supply in the baby (fetal hypoxia) early enough so that the baby can be delivered and not sustain permanent damage. For instance, it might be done if there is decreased fetal movement or a fetal growth problem, or your pregnancy goes past 42 weeks. But if your healthcare provider suggests a biophysical profile, it doesn’t mean anything is wrong with your baby. Your provider may have other reasons to recommend a biophysical profile.
The biophysical profile test is most commonly done when there’s an increased risk of problems that could lead to complications or pregnancy loss. Your health care provider will determine the necessity and timing of a biophysical profile based on whether your baby could survive if delivered early, the severity of your condition and the risk of pregnancy loss.
Your health care provider might initially recommend a modified biophysical profile — a simplified version of the test that includes a nonstress test and assesses amniotic fluid through ultrasound. He or she will use the results to determine whether you need a full biophysical profile, which also measures a baby’s breathing, movements and muscle tone, or other tests.
Your health care provider might recommend a biophysical profile if:
- You have a multiple pregnancy with certain complications
- You have a medical condition, such as diabetes, high blood pressure, lupus or heart disease
- Your pregnancy has extended two weeks past your due date (postterm pregnancy)
- You have a history of pregnancy loss or previous pregnancy complications
- Your baby has decreased fetal movements or possible fetal growth problems
- You have too much amniotic fluid (polyhydramnios) or a low amniotic fluid volume (oligohydramnios)
- You have rhesus (Rh) sensitization — a potentially serious condition that can occur when your blood group is Rh negative and your baby’s blood group is Rh positive
- You are older than age 35
- You are obese
Your health care provider might also recommend a biophysical profile if you’re between 40 and 42 weeks pregnant. The benefits of having the test done during this period, however, aren’t clear.
Your health care provider might recommend that you have a biophysical profile once a week or twice a week, depending on your health condition — until you deliver.
Biophysical profile score
Fetal biophysical profile score (BPS or BPP) refers to assessment of four discrete biophysical variables by ultrasound. It is a standard tool in antepartum fetal assessment. It is usually assessed after 28 weeks of gestation.
Each of the five components – body movements, muscle tone, breathing movements, amniotic fluid, and heartbeat – is assigned a score of either 0 (abnormal) or 2 (normal), depending on whether specific criteria were met. A score can be given immediately. For example:
- Fetal heart rate monitoring or CTG (cardiotocograph) test. This test checks your baby’s heart rate and your contractions. This is done through devices (sensors) that are strapped to belts wrapped around your belly. Nonstress means that nothing is done to cause your baby stress during the test. Results of this portion of the test (nonstress test) are interpreted as reactive or nonreactive. If your baby’s heartbeat accelerates twice or more a certain amount within a 20-minute period, the results are considered reactive and 2 points will be given. If not enough accelerations occur within a 40-minute period, the results are considered nonreactive and 0 points will be given. Keep in mind that nonreactive results might occur because your baby was asleep during the test.
- Fetal breathing. If your baby displays at least one episode of rhythmic breathing for 30 seconds or more within 30 minutes, 2 points will be given. If your baby’s breathing doesn’t meet the criteria, 0 points will be given.
- Fetal breathing is considered abnormal if there is:
- Absent breathing
- No breathing episode for ≥20 seconds within a 30 minute lapse
- Fetal breathing is considered abnormal if there is:
- Fetal movement. If your baby moves his or her body or limbs three times or more within 30 minutes, 2 points will be given. If your baby’s movements don’t meet the criteria, 0 points will be given.
- Fetal movement (gross body movement) is considered abnormal if there is: <2 episodes of body/limb movements within a 30 minute lapse
- Fetal muscle tone. If your baby moves a limb from a bent position to an extended position and quickly back to a bent position, 2 points will be given. If your baby’s muscle tone doesn’t meet the criteria, 0 points will be given.
- Fetal tone is considered abnormal if there is:
- Slow extension with return to partial flexion
- Absent fetal movement
- Fetal tone is considered abnormal if there is:
- Amniotic fluid level. The ultrasound technician will look for the largest visible pocket of amniotic fluid. To obtain a score of 2 points, the pocket must be a certain size. If your amniotic fluid level doesn’t meet the criteria, 0 points will be given.
- Amniotic fluid volume is considered abnormal if the largest pocket is <2 x 2 cm
The individual scores are then added together for a total score ranging from 0 to 10. Typically, a score of 8 to 10 is reassuring. If you receive a score of 6, your health care provider will likely repeat the test within 24 hours (you may be asked to have something to eat and come back for it to be reassessed) or, if your pregnancy is near term, delivery might be recommended. Umbilical arterial Doppler assessment is usually additionally carried out to evaluate fetuses with abnormal BPP scores. A BPP score of 4 or lower means that further testing is needed or that you might need to deliver the baby early or immediately.
In addition, if your health care provider finds that you have a low amount of amniotic fluid, you’ll need further testing and might need to deliver your baby early — regardless of your overall score.
Certain factors can affect the results of a biophysical profile, including the recent use of corticosteroids to speed your baby’s lung maturity. Taking certain medications, such as morphine, also can affect the score.
Be sure to discuss the results of your biophysical profile with your health care provider to fully understand what they might mean for you and your baby.
Table 1. Fetal Biophysical Profile Scoring
| Variable | Normal (Score = 2) | Abnormal (Score = 0) | |||
| Fetal breathing movements | 1 or more episodes of >20 s within 30 min | Absent or no episode of >20 s within 30 min | |||
| Body movements | 2 or more discrete body/ limb movements within 30 min (episodes of active continuous movement considered as a single movement) | <2 episodes of body/limb movements within 30 min | |||
| Fetal tone | 1 or more episodes of active extension with return to flexion of fetal limb(s) or trunk (opening and closing of hand considered normal tone) | Slow extension with return to partial flexion, movement of limb in full extension, absent fetal movement, or partially open fetal hand | |||
| Reactive fetal heart rate | 2 or more episodes of acceleration of >15 beats per minute* and of >15 seconds associated with fetal movement within 20 min | 1 or more episodes of acceleration of fetal heart rate or acceleration of <15 beats per minute within 20 min | |||
| Qualitative amniotic fluid volume | 1 or more pockets of fluid measuring >2 cm in vertical axis | Either no pockets or largest pocket <2 cm in vertical axis | |||
Footnotes:
- Amniotic Fluid Volume: Measured as the vertical measurement, in centimeters, of the single deepest pocket of amniotic fluid with a transverse measurement of 1 cm or more wide without fetal small parts or umbilical cord 1)
- * Reactive fetal heart rate: Two or more fetal heart rate accelerations that peak (but do not necessarily remain) at least 15 beats per minute above the baseline and last at least 15 seconds from baseline to baseline during 20 minutes of observation
- Nonreactive fetal heart rate: Less than two accelerations of fetal heart rate as described above after 40 minutes of observation 2)
Biophysical Profile Test Score Results
A total BPP score of 10 out of 10 or 8 out of 10 with normal fluid is considered normal. A score of 6 is considered equivocal, and a score of 4 or less is abnormal 3). A BPP score of less than 8 indicates the fetus may not be receiving enough oxygen. However, decreased biophysical activities may also be seen for a brief time in the preterm fetus after treatment with ether betamethasone or dexamethasone given to enhance fetal lung maturity 4).
Table 2. Biophysical Profile Test Score Results
| Test Score | Management | |
| American College of Obstetricians and Gynecologists 5) | Society of Obstetrics and Gynaecologists of Canada 6) | |
| 10 out of 10, 8 out of 10 (normal fluid), 8 out of 10 nonstress test (NST) not done | Deliver for obstetric or maternal factors | |
| 8 out of 10 (abnormal fluid) | Uncomplicated, isolated persistent oligohydramnios deliver at 36 to 37 weeks. | If there is normal urinary tract function and intact membranes then deliver at term. If < 34 weeks intensive surveillance to maximize maturity |
| 6 out of 10 (normal fluid) | At or beyond 37 weeks of gestation, further evaluation and consideration of delivery. Less than 37 weeks repeat BPP in 24 hours | Repeat test within 24 hours |
| 6 out of 10 (abnormal fluid) | At or beyond 37 weeks of gestation, further evaluation and consideration of delivery. Less than 37 weeks repeat BPP in 24 hours | Deliver if at term .If < 34 weeks intensive surveillance to maximize maturity |
| 4 out of 10 | Delivery is usually indicated. Pregnancies at less than 32 weeks of gestation, management should be individualized, and extended monitoring may be appropriate. | Deliver |
| 2 out of 10 | Deliver | Deliver |
| 0 out of 10 | Deliver | Deliver |
How reliable is the biophysical profile score?
The biophysical profile (BPP) is a fairly reliable method of predicting fetal survival. Data have been collected on this and other ante-partum testing procedures for more than 20 years.
Testing methods usually are evaluated by comparing the false-negative mortality rate for each method.
The false-negative mortality rate is defined as the number of fetal deaths, corrected for lethal congenital anomalies and unpredictable causes of demise, that occur within 1 week of a normal test result.
The biophysical profile (BPP) has a false-negative mortality rate of 0.77 deaths per 1000 tests.
Furthermore, the score correlates well with the fetal umbilical venous cord pH level and neonatal outcomes.
If you would like more information, please talk to your doctor or midwife or the obstetricians when you have your test.
Biophysical profile test risks
The biophysical profile is an easy, safe, and painless procedure. A biophysical profile is a noninvasive test that poses no physical risks to you or your baby. Some concern has been raised about doing ultrasounds over a long period of time. But having an ultrasound now and then doesn’t seem to be a risk to your baby. A biophysical profile typically requires no special preparation. However, some reports show maternal fasting resulting in reduced fetal breathing movements which can in turn affect the biophysical profile score (BPP score) 7).
For the nonstress test, the provider wraps 2 belts are wrapped around your belly. Devices (sensors) attached to these belts will check your baby’s heart rate and your contractions. For the ultrasound, the provider will put a gel on your belly. Then he or she will move an ultrasound wand (transducer) and press into the gel. This will give a view into your uterus. The images can be seen on a screen.
While a biophysical profile can offer reassurance about your baby’s health, it can also cause anxiety. In addition, a biophysical profile might not detect an existing problem or might suggest that a problem exists when there is none. A test that falsely indicates a problem might cause your health care provider to recommend unnecessary tests or early delivery.
Also, keep in mind that it’s not always clear that the biophysical profile test can improve pregnancy outcomes.
Be sure to talk with your healthcare provider about any concerns you have before the test.
Biophysical profile test procedure
A biophysical profile can be done in your health care provider’s office or in a hospital. The test might take 30 minutes or so to complete. A modified biophysical profile takes less time.
Generally a biophysical profile follows this process:
- Your provider will explain the test to you. Ask him or her any questions you have about the test.
- You may be asked to undress and put on a hospital gown.
- You will lie down on an exam table or bed.
- The nonstress test is often done first. The provider puts a belt with a device (sensor) attached around your belly. The sensor checks your baby’s heart rate. This will be displayed on a screen.
- The provider puts a second belt and sensor around you right next to the first. This sensor measures your contractions. Even though labor may still be a few weeks off, contractions are normal at this point in your pregnancy. This part of the test often lasts 20 to 30 minutes.
- If your baby doesn’t move during the test, don’t panic. The baby might be asleep. If this happens, a nurse may try to wake the baby with a buzzer.
- The belts and devices are then taken off. This part of the test is over.
- The ultrasound part of the test may take up to 1 hour. Your provider will put warmed ultrasound gel on your bare belly.
- The provider will press a small, handheld wand (transducer) into the gel and against your belly. Images of your baby in your uterus will be shown on a screen.
- The provider will look at your baby’s breathing movements, body movement, and muscle tone. He or she will also measure the amniotic fluid around the baby.
- When this part of the exam is complete, the provider will wipe the ultrasound gel off your belly. You can get dressed.
During the procedure
During the nonstress test, you’ll lie on an exam table and have a belt placed across your abdomen. The belt contains a sensor that measures the fetal heart rate. The heart rate is recorded by a machine. If your baby is asleep, you might need to wait until he or she awakens to ensure accurate results. In some cases, your health care provider might try to awaken the baby by projecting a sound over your abdomen.
During the ultrasound exam, you’ll also lie on an exam table. Your health care provider or an ultrasound technician will apply a small amount of gel to your abdomen. Then he or she will roll a small device called a transducer over your skin. The transducer will emit pulses of sound waves that will be translated into a pattern of light and dark areas — creating an image of your baby on a monitor.
Your health care provider or the ultrasound technician will then evaluate your baby’s breathing movements, body movements, muscle tone and amniotic fluid level. If your baby is asleep, this portion of the test might take a little longer.
After the procedure
When the biophysical profile is complete, your health care provider will likely discuss the results with you right away.
Modified Biophysical Profile
Some testing centers use a modified biophysical profile (MBPP) 8). The modified BPP consists of the nonstress test (NST) and an amniotic fluid volume assessment. The modified BPP is considered normal if the NST is reactive and the deepest vertical pocket of amniotic fluid is greater than 2 centimeters. The modified BPP is considered abnormal if either the nonstress test is nonreactive or the deepest vertical pocket of amniotic fluid is 2 cm or less 9).
When is the modified biophysical profile usually performed?
The modified biophysical profile may be performed for decreased fetal movement. If the nonstress test is nonreactive or the amniotic fluid volume is low a full biophysical profile is usually done.
The American College of Obstetricians and Gynecologists 10) recommends the modified biophysical profile or BPP may also be used for antepartum fetal surveillance in pregnancies at increased risk for bad perinatal outcomes including, but not limited to, pregnancies complicated by hypertension, preeclampsia, pregestational diabetes, poorly controlled or medically treated gestational diabetes, poorly controlled hyperthyroidism, chronic renal disease, systemic lupus erythematosus, antiphospholipid syndrome, hemoglobinopathy (sickle cell disease), maternal cyanotic heart disease, moderate or severe asthma during pregnancy, isoimmunization, oligohydramnios, unexplained or recurrent risk for stillbirth, fetal growth restriction , and late term pregnancy at or beyond 41 weeks 11).
The Society of Obstetricians and Gynaecologists of Canada 12) suggests antenatal fetal surveillance may also be beneficial in pregnancies complicated by preterm premature rupture of membranes, chronic (stable abruption), vaginal bleeding, abnormal maternal serum screening in the absence of confirmed fetal anomaly, motor vehicle accident during pregnancy, morbid obesity, advanced maternal age, assisted reproductive technologies , multiple pregnancy, polyhydramnios, and preterm labor 13).
In addition to many of the above indications an executive summary by a Eunice Kennedy Shriver National Institute of Child Health and Human Development workshop on antenatal testing suggested antepartum testing for cholestasis of pregnancy was appropriate 14). However, the workshop found insufficient data to recommend antenatal testing for other conditions such as obesity, advanced maternal age, abnormal maternal serum markers, thrombophilias, triplets and higher-order multiples 15).
The American College of Obstetricians and Gynecologists has observed that despite a lack of high quality evidence that antepartum surveillance decreases the risk of fetal death …”antepartum fetal surveillance is widely integrated into clinical practice in the developed world” 16). The American College of Obstetricians and Gynecologists advises “… initiating antepartum fetal testing no earlier than 32 0/7 weeks of gestation is appropriate for most at-risk patients. However, in pregnancies with multiple or particularly worrisome high-risk conditions (e.g., chronic hypertension with suspected fetal growth restriction), testing might begin at a gestational age when delivery would be considered for perinatal benefit”. If delivery is not planned (eg, given early gestational age), then antenatal surveillance should not be performed because the results will not inform management 17).
References [ + ]