Contents
What is shellfish allergy
Shellfish is one of the more common food allergies. Shellfish allergy usually is lifelong. About 60 percent of people with shellfish allergy experience their first allergic reaction as adults. If you have shellfish allergy, your immune system overreacts to a particular protein found in that shellfish. Shellfish allergy can develop at any age. Even people who have eaten shellfish in the past can develop an allergy. Some people outgrow certain food allergies over time, but those with shellfish allergies usually have the allergy for the rest of their lives.
There are two groups of shellfish:
- Crustacea (such as shrimp, crab and lobster) and
- Mollusks (such as clams, mussels, oysters, scallops, octopus and squid).
Most people with one shellfish allergy are allergic to other species within the same class. For example, if you are allergic to crab, you may also be allergic to lobster, shrimp and other crustaceans. Likewise, if you are allergic to clams, you may also be allergic to other mollusks, such as mussels or scallops.
Crustacea cause most shellfish reactions, and these tend to be severe. Shellfish allergic reactions can range from mild symptoms — such as hives or a stuffy nose — to severe and even life-threatening.
A shellfish allergy is not exactly the same as a seafood allergy. Seafood includes fish (like tuna or cod) and shellfish (like lobster or clams). Even though they both fall into the category of “seafood,” fish and shellfish are biologically different. So fish will not cause an allergic reaction in someone with a shellfish allergy, unless that person also has a fish allergy.
- Finned fish and shellfish are not related. Being allergic to one does not always mean that you must avoid both.
Carrageenan, or “Irish moss,” is not shellfish. It is a red marine algae used as an emulsifier, stabilizer and thickener in many foods like dairy foods. It is safe for most people with food allergies.
Shellfish allergy is sometimes confused with iodine allergy because shellfish is known to contain the element iodine. But iodine is not what triggers the reaction in people who are allergic to shellfish. If you have a shellfish allergy, you do not need to worry about cross-reactions with iodine or radiocontrast material (which can contain iodine and is used in some radiographic medical procedures).
Another misconception is that shellfish-allergic patients cannot take glucosamine. Glucosamine is normally safe to consume because it is made from shells, not the protein that causes allergy to shellfish.
Shellfish can cause severe and potentially life-threatening allergic reactions (such as anaphylaxis). Allergic reactions can be unpredictable, and even very small amounts of shellfish can cause one. Most allergic reactions to shellfish happen when someone eats shellfish, but sometimes a person can react to touching shellfish or breathing in vapors from cooking shellfish.
If you have a shellfish allergy, keep an epinephrine auto-injector (such as an EpiPen®, Auvi-Q™ or Adrenaclick®) with you at all times. Epinephrine is the first-line treatment for anaphylaxis.
To prevent a reaction, it is very important to avoid all shellfish and shellfish products. Always read food labels and ask questions about ingredients before eating a food that you have not prepared yourself.
Most people who are allergic to one group of shellfish are allergic to other types. Your allergist will usually recommend you avoid all kinds of shellfish. If you are allergic to a specific type of shellfish but want to eat other shellfish, talk to your doctor about further allergy testing.
Steer clear of seafood restaurants, where there is a high risk of food cross-contact. You should also avoid touching shellfish and going to fish markets. Being in any area where shellfish are being cooked can put you at risk, as shellfish protein could be in the steam.
Shellfish is one of the eight major allergens that must be listed on packaged foods sold in the U.S., as required by federal law. However, mollusks are not considered major allergens under food labeling laws and may not be fully disclosed on a product label.
Many people who think they are allergic to shellfish may actually be intolerant to it. Some of the symptoms of food intolerance and food allergy are similar, but the differences between the two are very important. An intolerance to shellfish can make you feel miserable. An allergy to shellfish can result in symptoms of anaphylaxis, a life-threatening allergic reaction.
An allergist / immunologist has advanced training and experience to determine if you are intolerant or allergic to shellfish and help you manage your condition.
What Happens in a Shellfish Allergy
When someone is allergic to shellfish, the body’s immune system, which normally fights infections, overreacts to proteins in the shellfish. Every time the person eats (or, in some cases, handles or breathes in) shellfish, the body thinks these proteins are harmful invaders.
The immune system responds by working very hard to fight off the invader. This causes an allergic reaction, in which chemicals like histamine are released in the body. The release of these chemicals can cause someone to have these symptoms:
- wheezing
- trouble breathing
- coughing
- hoarseness
- throat tightness
- stomachache
- vomiting
- diarrhea
- itchy, watery, or swollen eyes
- hives
- red spots
- swelling
- a drop in blood pressure causing lightheadedness or loss of consciousness
Your could have different reactions to different types of shellfish or react differently at different times. Some reactions can be very mild and involve only one system of the body, like hives on the skin. Other reactions can be more severe and involve more than one part of the body.
What is anaphylaxis
Anaphylaxis is a severe and potentially life-threatening reaction to a trigger such as an allergy. It’s also known as anaphylactic shock.
- Anaphylaxis is a medical emergency that requires immediate medical assistance and treatment.
- Anaphylaxis can occur within seconds or minutes of exposure to something you’re allergic to, such as peanuts or bee stings.
Anaphylaxis causes your immune system to release a flood of chemicals that can cause you to go into shock — your blood pressure drops suddenly and your airways narrow, blocking breathing. Signs and symptoms include a rapid, weak pulse; a skin rash; and nausea and vomiting. Common triggers include certain foods, some medications, insect venom and latex.
Anaphylaxis requires an injection of epinephrine and a follow-up trip to an emergency room. If you don’t have epinephrine, you need to go to an emergency room immediately. If anaphylaxis isn’t treated right away, it can be fatal.
- Trouble breathing or noisy breathing
- Difficulty talking more than a few words and/or hoarse voice
- Wheeze
- Cough
- Swelling and tightness of the throat
- Collapse
- Light-headedness or dizziness
- Diarrhea
- Tingling in the hands, feet, lips or scalp
- Swelling of tongue
- Pale and floppy (in young children)
A severe allergic reaction (anaphylaxis) is a medical emergency. Call your local emergency immediately. Lay the person down. If they have an adrenaline injector and you are able to administer it, do so.
Anaphylaxis is a medical emergency. It can be very serious if not treated quickly.
If someone has symptoms of anaphylaxis, you should:
- Call your local emergency number for an ambulance immediately – mention that you think the person has anaphylaxis
- Remove any trigger if possible – for example, carefully remove any wasp or bee sting stuck in the skin
- Lie the person down flat and elevate his or her legs – unless they’re unconscious, pregnant or having breathing difficulties
- Use an adrenaline auto-injector if the person has one – but make sure you know how to use it correctly first
- Check the person’s pulse and breathing and, if necessary, administer CPR (cardiopulmonary resuscitation) or other first-aid measures
- Give another injection after 5-15 minutes if the symptoms don’t improve and a second auto-injector is available
If you’re having an anaphylactic reaction, you can follow these steps yourself if you feel able to.
How to use Adrenaline auto-injectors
People with potentially serious allergies will often be given an adrenaline auto-injector to carry at all times. This can help stop an anaphylactic reaction becoming life threatening.
This should be used as soon as a serious reaction is suspected, either by the person experiencing anaphylaxis or someone helping them.
If you’ve been given an auto-injector, make sure you’re aware how to use it correctly.
There are three main types of adrenaline auto-injector, which are used in slightly different ways.
These are:
- EpiPen – see Figure 1 on how to use Epipen
- Jext
- Emerade
Instructions are also included on the side of each injector if you forget how to use it or someone else needs to give you the injection.
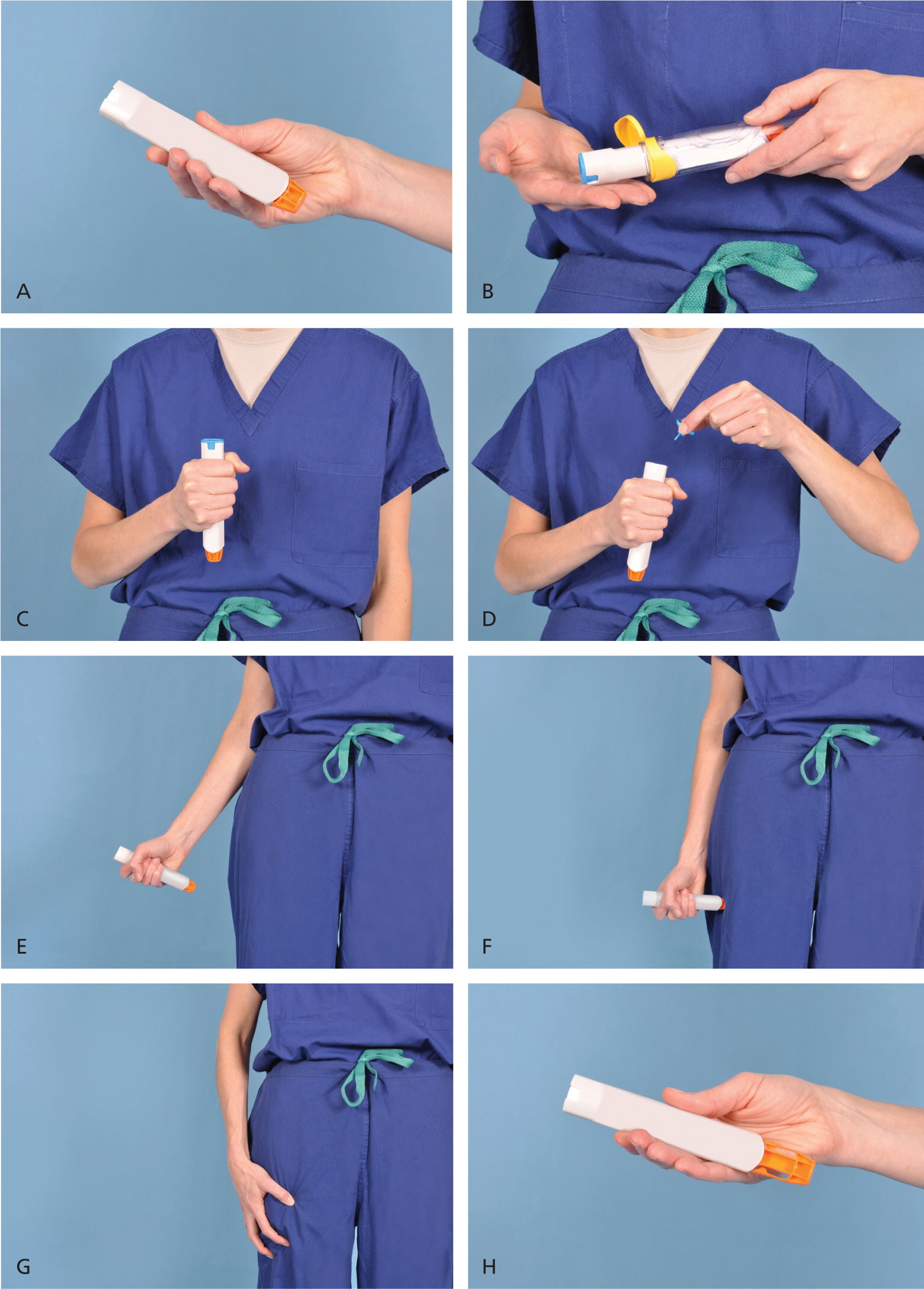
Figure 1. How to use the Epipen
Demonstration of appropriate deployment of the (A) Epipen (released in 2008). For demonstration purposes, a trainer device is being used instead of a live device; however, the coloring of key components is the same as the actual adult device. (B) Open the yellow cap of the carrying case and remove the device from its storage tube (the Epipen Jr. has a green cap). (C) Grasp and form a fist around the unit with the orange tip facing down. (D) With the other hand, remove the blue safety release. (E) Aim the orange tip toward the outer thigh. (F) Swing the arm and jab the device firmly into the outer thigh, at a 90-degree angle, until the device clicks. The needle will deploy at this time into thigh (the autoinjector is designed to work through clothing). Hold the device firmly against the thigh for 10 seconds, so the entire dose will be delivered. (G) Remove the device from the thigh and massage the injection area for 10 seconds. (H) The safety feature of the device, extension of the orange tip that locks into place, will completely cover the needle immediately after use. The used device should be taken to the hospital emergency department with the patient for disposal.
Positioning and resuscitation
Someone experiencing anaphylaxis should be placed in a comfortable position.
- Most people should lie flat.
- Pregnant women should lie on their left side to avoid putting too much pressure on the large vein that leads to the heart.
- People having trouble breathing should sit up to help make breathing easier.
- People who are unconscious should be placed in the recovery position to ensure the airway remains open and clear – place them on their side, making sure they’re supported by one leg and one arm, and open their airway by lifting their chin.
- Avoid a sudden change to an upright posture such as standing or sitting up – this can cause a dangerous fall in blood pressure.
If the person’s breathing or heart stops, cardiopulmonary resuscitation (CPR) should be performed immediately.
How to perform a Cardiopulmonary Resuscitation (CPR)
Hands-only CPR
To carry out a chest compression:
- Place the heel of your hand on the breastbone at the centre of the person’s chest. Place your other hand on top of your first hand and interlock your fingers.
- Position yourself with your shoulders above your hands.
- Using your body weight (not just your arms), press straight down by 5-6cm (2-2.5 inches) on their chest.
- Keeping your hands on their chest, release the compression and allow the chest to return to its original position.
- Repeat these compressions at a rate of 100 to 120 times per minute until an ambulance arrives or you become exhausted.
When you call for an ambulance, telephone systems now exist that can give basic life-saving instructions, including advice about CPR. These are now common and are easily accessible with mobile phones.
Cardiopulmonary Resuscitation (CPR) with rescue breaths
If you’ve been trained in CPR, including rescue breaths, and feel confident using your skills, you should give chest compressions with rescue breaths. If you’re not completely confident, attempt hands-only CPR instead (see above).
Adults
- Place the heel of your hand on the centre of the person’s chest, then place the other hand on top and press down by 5-6cm (2-2.5 inches) at a steady rate of 100 to 120 compressions per minute.
- After every 30 chest compressions, give two rescue breaths.
- Tilt the casualty’s head gently and lift the chin up with two fingers. Pinch the person’s nose. Seal your mouth over their mouth and blow steadily and firmly into their mouth for about one second. Check that their chest rises. Give two rescue breaths.
- Continue with cycles of 30 chest compressions and two rescue breaths until they begin to recover or emergency help arrives.
Children over one year old
- Open the child’s airway by placing one hand on the child’s forehead and gently tilting their head back and lifting the chin. Remove any visible obstructions from the mouth and nose.
- Pinch their nose. Seal your mouth over their mouth and blow steadily and firmly into their mouth, checking that their chest rises. Give five initial rescue breaths.
- Place the heel of one hand on the center of their chest and push down by 5cm (about two inches), which is approximately one-third of the chest diameter.
- The quality (depth) of chest compressions is very important. Use two hands if you can’t achieve a depth of 5cm using one hand.
- After every 30 chest compressions at a rate of 100 to 120 per minute, give two breaths.
- Continue with cycles of 30 chest compressions and two rescue breaths until they begin to recover or emergency help arrives.
Infants under one year old
- Open the infant’s airway by placing one hand on their forehead and gently tilting the head back and lifting the chin. Remove any visible obstructions from the mouth and nose.
- Place your mouth over the mouth and nose of the infant and blow steadily and firmly into their mouth, checking that their chest rises. Give five initial rescue breaths.
- Place two fingers in the middle of the chest and push down by 4cm (about 1.5 inches), which is approximately one-third of the chest diameter. The quality (depth) of chest compressions is very important. Use the heel of one hand if you can’t achieve a depth of 4cm using the tips of two fingers.
- After 30 chest compressions at a rate of 100 to 120 per minute, give two rescue breaths.
- Continue with cycles of 30 chest compressions and two rescue breaths until they begin to recover or emergency help arrives.
Recovery position
If a person is unconscious but is breathing and has no other life-threatening conditions, they should be placed in the recovery position.
Putting someone in the recovery position will keep their airway clear and open. It also ensures that any vomit or fluid won’t cause them to choke.
Figure 2. Recovery position
The video shows a step-by-step guide to putting someone in the recovery position.
Or you can follow these steps:
- with the person lying on their back, kneel on the floor at their side
- place the arm nearest you at a right angle to their body with their hand upwards, towards the head
- tuck their other hand under the side of their head, so that the back of their hand is touching their cheek
- bend the knee farthest from you to a right angle
- carefully roll the person onto their side by pulling on the bent knee
- the top arm should be supporting the head and the bottom arm will stop you rolling them too far
- open their airway by gently tilting their head back and lifting their chin, and check that nothing is blocking their airway
- stay with the person and monitor their condition until help arrives.
Figure 3. Anaphylaxis Emergency Action Plan
For a Shellfish-Free Diet
*Note: The federal government does not require mollusks to be fully disclosed on product labels.
Avoid foods that contain shellfish or any of these ingredients:
- Barnacle
- Crab
- Crawfish (crawdad, crayfish, ecrevisse)
- Krill
- Lobster (langouste, langoustine, Moreton bay bugs, scampi, tomalley)
- Prawns
- Shrimp (crevette, scampi)
Shellfish are sometimes found in the following:
- Bouillabaisse
- Cuttlefish ink
- Glucosamine
- Fish stock
- Seafood flavoring (e.g., crab or clam extract)
- Surimi
Your may want to avoid mollusks or these ingredients:
- Abalone
- Clams (cherrystone, geoduck, littleneck, pismo, quahog)
- Cockle
- Cuttlefish
- Limpet (lapas, opihi)
- Mussels
- Octopus
- Oysters
- Periwinkle
- Sea cucumber
- Sea urchin
- Scallops
- Snails (escargot)
- Squid (calamari)
- Whelk (Turban shell)
Keep the following in mind:
- Any food served in a seafood restaurant may contain shellfish protein due to cross-contact.
- For some individuals, a reaction may occur from inhaling cooking vapors or from handling fish or shellfish.
Carrageenan, or “Irish moss,” is not shellfish. It is a red marine algae used as an emulsifier, stabilizer and thickener in many foods like dairy foods. It is safe for most people with food allergies.
Shellfish allergy is sometimes confused with iodine allergy because shellfish is known to contain the element iodine. But iodine is not what triggers the reaction in people who are allergic to shellfish. If you have a shellfish allergy, you do not need to worry about cross-reactions with iodine or radiocontrast material (which can contain iodine and is used in some radiographic medical procedures).
What causes shellfish allergy
All food allergies are caused by an immune system overreaction. Your immune system identifies a certain shellfish protein as harmful, triggering the production of antibodies to the shellfish protein (allergen). The next time you come in contact with the allergen, your immune system releases histamine and other chemicals that cause allergy symptoms.
Types of shellfish
There are several types of shellfish, each containing different proteins:
- Crustaceans include crabs, lobster, crayfish, shrimp and prawn.
- Mollusks include squid, snails, octopus, clams, oysters and scallops.
Some people are allergic to only one type of shellfish but can eat others. Other people with shellfish allergy must avoid all shellfish.
Risk factors for shellfish allergy
You’re at increased risk of developing a shellfish allergy if allergies of any type are common in your family.
Though people of any age can develop a shellfish allergy, it’s more common in adults. Among adults, shellfish allergy is more common in women. Among children, shellfish allergy is more common in boys.
Shellfish allergy prevention
If you have a shellfish allergy, the only way to avoid an allergic reaction is to avoid all shellfish and products that contain shellfish. Even trace amounts of shellfish can cause a severe reaction in some people.
Avoiding shellfish
- Be cautious when dining out. When dining at restaurants, always check to make sure that the pan, oil or utensils used for shellfish aren’t also used to prepare other foods, creating cross-contamination. It might be necessary to avoid eating at seafood restaurants, where there’s a high risk of cross-contamination.
- Read labels. Cross-contamination can occur in stores where other food is processed or displayed near shellfish and during manufacturing. Read food labels carefully. Shellfish is rarely a hidden ingredient, but it may be in fish stock or seafood flavoring. Companies are required to label any product that contains shellfish or other foods that often cause allergic reactions, but the regulations don’t apply to mollusks, such as clams, oysters and scallops.
- Keep your distance. You may need to completely avoid places where shellfish are prepared or processed. Some people react after touching shellfish or inhaling steam from cooking shellfish.
If you have a shellfish allergy, talk with your doctor about carrying emergency epinephrine. Consider wearing a medical alert bracelet or necklace that lets others know you have a food allergy.
It’s untrue that people with shellfish allergy also will be allergic to iodine or radiocontrast dye used in some lab procedures. Reactions to radiocontrast material or iodine aren’t related.
Shellfish Allergy Safety Tips
To prevent allergic reactions, your child must not eat shellfish. He or she also must not eat any foods that might contain shellfish as ingredients. For detailed information, visit food allergy websites, such as the Food Allergy Research and Education 1) or others that your doctor recommends.
Also, read food labels to see if a food is free of shellfish. Makers of foods sold in the United States must state in understandable language whether foods contain any of the top eight most common allergens, including crustacean shellfish. The label should list “shellfish” in the ingredient list or say “Contains shellfish” after the list.
Also look for advisory statements such as “May contain shellfish,” “Processed in a facility that also processes shellfish,” or “Manufactured on equipment also used for shellfish.” These are cross-contamination warnings, but manufacturers are not required to list them.
Because products without precautionary statements also might be cross-contaminated and the company simply chose not to label for it, it is always best to contact the company to see if the product could contain shellfish. You might find this information on the company’s website or you can email a company representative.
Manufacturers also do not have to list mollusk shellfish ingredients because mollusk shellfish (clams, mussels, oysters, or scallops) are not considered a major food allergen. When labels say a food contains shellfish, they refer to crustacean shellfish. Contact the company to see about cross-contamination risk with mollusks.
Even if a food did not cause a reaction in the past, it still could be a problem. Manufacturers may change processes or ingredients at any time.
Shellfish ingredients also might be used in some non-food products, like nutritional supplements, lip gloss, pet foods, and plant fertilizer. Talk to your doctor if you have questions about what is safe.
Cross-Contamination
Cross-contamination is common in restaurants, which is where many people often mistakenly eat shellfish. This happens in kitchens when shellfish gets into a food product because the staff use the same surfaces, utensils (like knives, cutting boards, or pans), or oil to prepare both shellfish and other foods.
This is particularly common in seafood restaurants, so some people find it safer to simply avoid these restaurants altogether. Since shellfish is also used in a lot of Asian cooking, there’s a risk of cross-contamination in Chinese, Vietnamese, Thai, or Japanese restaurants. It’s a good idea to avoid a restaurant’s fried foods, like French fries and fried chicken, because the restaurant may use the same oil to fry shrimp.
Eating Away From Home
When you eat in a restaurant or at a friend’s house, find out how foods are cooked and exactly what’s in them. It can be hard to ask a lot of questions about cooking methods, and to trust the information you get. If you can’t be certain that a food is shellfish-free, it’s best to bring safe food from home.
Also talk to the staff at school about cross-contamination risks for foods in the cafeteria. It may be best to pack lunches at home so you can control what’s in them.
If you are eating at a restaurant, take these precautions:
- Stay away from steam tables or stove tops when shellfish is cooked (especially places where food is cooked on a communal grill, like hibachi restaurants).
- Tell the restaurant waitstaff that your child has as serious shellfish allergy.
- Carry a personalized “chef card” for your child, which can be given to the kitchen staff. The card details your child’s allergies for food preparers. Food allergy websites provide printable chef card forms in many different languages 2).
- Don’t eat at a restaurant if the manager or owner seems uncomfortable about your requests for a safe meal.
Figure 4. Chef card
How to use your chef card:
In addition to asking a lot of questions about the ingredients and preparation methods, carry a “chef card” that outlines the foods you must avoid. Present the card to the chef or manager for review.
Fold your card in half, then tape it together and store in your wallet. You can even laminate it to make it more durable. Be sure to make several copies in case you forget to retrieve it from the restaurant or to store in multiple locations.
Shellfish allergy signs and symptoms
Shellfish allergy symptoms generally develop within minutes to an hour of eating shellfish. They may include:
- Hives, itching or eczema (atopic dermatitis)
- Swelling of the lips, face, tongue and throat, or other parts of the body
- Wheezing, nasal congestion or trouble breathing
- Abdominal pain, diarrhea, nausea or vomiting
- Dizziness, lightheadedness or fainting
- Tingling in the mouth
Allergies can cause a severe, potentially life-threatening reaction known as anaphylaxis. An anaphylactic reaction to shellfish or anything else is a medical emergency that requires treatment with an epinephrine (adrenaline) injection and a trip to the emergency room.
Signs and symptoms of anaphylaxis include:
- A swollen throat or a lump in your throat (airway constriction) that makes it difficult for you to breathe
- Shock, with a severe drop in your blood pressure
- Rapid pulse
- Dizziness, lightheadedness or loss of consciousness
Shellfish allergy complications
In severe cases, shellfish allergy can lead to anaphylaxis, a dangerous allergic reaction marked by a swollen throat (airway constriction), rapid pulse, shock, and dizziness or lightheadedness. Anaphylaxis can be life-threatening.
When you have shellfish allergy, you may be at increased risk of anaphylaxis if:
- You have asthma
- You have allergic reactions to very small amounts of shellfish (extreme sensitivity)
- You have a history of food-induced anaphylaxis
Anaphylaxis can be treated with an emergency injection of epinephrine (adrenaline). If you are at risk of having a severe allergic reaction to shellfish, you always should carry injectable epinephrine (EpiPen, Auvi-Q, others).
Shellfish allergy diagnosis
Your doctor will ask about your symptoms and may perform a physical exam to find or rule out other medical problems. He or she may also recommend one or both of the following tests:
- Skin test. In this test, your skin is pricked and exposed to small amounts of the proteins found in shellfish. If you’re allergic, you’ll develop a raised bump (hive) at the test site on your skin.
- Blood test. Also called allergen-specific IgE antibody test or radioallergosorbent (RAST) test, this test can measure your immune system’s response to shellfish proteins by measuring the amount of certain antibodies in your bloodstream, known as immunoglobulin E (IgE) antibodies.
A history of allergic reactions shortly after exposure to shellfish can be a sign of a shellfish allergy, but allergy testing is the only sure way to tell what’s causing your symptoms and to rule out other possibilities, such as food poisoning.
Shellfish allergy treatment
The only sure way to prevent an allergic reaction to shellfish is to avoid shellfish. But despite your best efforts, you may come into contact with shellfish.
Your doctor may instruct you to treat a mild allergic reaction to shellfish, with medications such as antihistamines to reduce signs and symptoms, such as rash and itchiness.
If you have a severe allergic reaction to shellfish (anaphylaxis), you’ll likely need an emergency injection of epinephrine (adrenaline). If you’re at risk of having a severe reaction, carry injectable epinephrine (EpiPen, Auvi-Q, others) with you at all times. If you’re at risk for anaphylaxis to shellfish, your doctor may instruct you to administer epinephrine even at the first sign of an allergic reaction. After you use epinephrine, seek emergency medical care.
References [ + ]